
Issue Paper

Future Nursing Facility Funding Concerns
Background:
Wisconsin nursing facilities are facing a funding and staffing crisis that must be addressed. Every day facilities confront multiple issues that effect the lives of tens of thousands of residents, families and staff. These facilities are struggling under increasingly difficult circumstances to deliver the highest quality of care and services expected and demanded of them. WAHSA member facilities are greatly appreciative of the Legislature's efforts to fund the wage pass-through for certified nursing assistants (CNAs) under 1999 Wisconsin Act 9, the 1999-01 biennial budget. Indeed, we are seeking additional legislation to provide a 3.5% wage pass-through for nursing home housekeepers, food workers and laundry workers. That appreciation, however, cannot mask the fact that a wage pass-through is only a short-term solution to a long-term problem. As detailed below, we believe future substantial Medicaid nursing facility payment increases are necessary to ensure quality nursing facility care.
This paper discusses some of the challenges of providing nursing home care, explains many of the factors that drive long term care facility costs, and asks the Legislature to support a permanent and stable funding solution as part of the 2001-03 biennial budget bill.
Why Are Nursing Facility Costs Increasing?
Resident Needs Are More Complex
Nursing home costs continue to escalate due to a rapid rise in the medical and behavioral needs of their residents. As shown in Graph #1, the number of nursing home residents in need of higher and more costly skilled nursing or intensive skilled nursing levels of care (SNF/ISN) at the time of admission has increased from 79.4% in 1988 to 97% in 1998. Today, fewer than three percent of nursing home residents require the lower intermediate level of care (ICF) at the time of admission.

Also, nursing home residents of today exhibit many more medical and behavioral symptoms than a decade ago. This stands to reason since nearly eighty percent of all skilled nursing facility admissions come directly from an acute care hospital. While today's nursing facility resident has significant and costly care and service needs, facilities are doing an excellent job of providing restorative and rehabilitative care, enabling over forty-percent of nursing home residents discharged to return to a private residence. For most facilities, the average length of stay for a nursing facility admission is measured in days or weeks. As shown in Graph #2, although the annual census of Wisconsin nursing facilities has decreased since 1990 by some 3,300 residents, the number of annual admissions since 1990 has increased by over 24,500, or a 93% increase.

Increasing admissions also increase costs. Each nursing facility admission triggers a very staff-intensive process. Federal regulations mandate facilities to expeditiously complete for every resident a detailed and comprehensive assessment and produce a written resident-specific plan of care. This plan of care must be constantly updated and documented and the resident data must be entered into a computer database that is sent to the state and federal survey agencies. Thus, while it is the goal of nursing facilities to return residents to their traditional home, when possible, the significant increase in admissions concomitantly has increased nursing facility costs as facilities have been forced to add nursing assessment, data entry and documentation staff.
Nursing Facilities Face a Staffing Crisis
Without question, Wisconsin's nursing facilities face a mounting staffing crisis. Within the past twelve months, seventeen facilities reported having to deny admissions because of the lack of staff. According to a 1999 survey jointly conducted by the nursing facility provider associations: 75% of the homes reported a "significantly more difficult" time attracting workers than two years ago (38.5% responded "significantly worse"); on average 13.8% of budgeted CNA positions were vacant; and staff turnover rates continue to rise. Working in a long-term care setting is rewarding and inspirational work; it is also very demanding and often times stressful. Because Medicaid is the primary payment source for nearly 70% of all nursing home residents, the ability of facilities to adequately compensate staff is frequently hamstrung by inadequate Medicaid reimbursement rates. There is a direct correlation between wages, benefits and staffing hours (i.e., employees assigned to resident cares) and a facility's staff turnover rate. As shown by Graph #3, facilities that offer relatively higher employee compensation packages and staffing hours generally have greater success in reducing their CNA turnover.

The significance of the correlation between turnover rates and quality of care was noted in a report published in 1994 by the Department of Health and Family Services (DHFS) Center for Health Statistics: "One important aspect of quality of care in nursing homes is the continuity of employment among the nursing staff. Low continuity can lead to staff shortages, which in turn allows less time for resident care. A time lag usually occurs between the date an employee leaves a facility and the date a replacement begins work. Training of new employees also absorbs time. Therefore, it can generally be assumed that the lower the nursing home turnover rate, the better the quality of care will be."
Why Are Current Medicaid Funding Levels Inadequate?
According to figures recently released by the Legislative Audit Bureau in an audit of county nursing home funding ("An Evaluation: County Nursing Home Funding" - Department of Health and Family Services - 00-1 - January 2000), the State provided $698.1 million in state and federal Medicaid funding in FY 1998-99 for Medical Assistance recipients requiring skilled care in 417 Wisconsin nursing facilities. Despite this seeming generosity, this paper seeks to outline the factors which WAHSA members believe render this funding level inadequate.
Elimination of the "Boren Amendment"
In 1997, Congress repealed the "Boren Amendment," which required States to reimburse nursing facilities at levels that are "reasonable and adequate to meet the costs that must be incurred by efficiently and economically operated providers." Congress estimates repeal of the "Boren Amendment" will generate a savings of $1.2 billion over five years. Since previous rate increases for nursing homes were provided in part to ensure compliance with the "Boren Amendment," its elimination, coupled with the savings projected to be generated by that elimination, removes an important protection against inadequate nursing home funding.
Medicaid Rates Don't Meet Inflation
1999 Wisconsin Act 9 included a 2.5% Medicaid rate increase for nursing homes in FY 1999-00 and a 2% increase in FY 00-01. Those increases are less than the 3.4% increase in nursing facility costs estimated by the DHFS for that time period. The result: Despite a 2.5% rate increase for July 1, 1999 - June 30, 2000, 140 of the 154 nursing facilities in the WAHSA database, or 91%, will incur aggregate Medicaid costs that are $66.7 million greater than their Medicaid reimbursement. That Medicaid deficit figure would have been closer to $102 million if it were not for the $35.3 million in intergovernmental transfer (IGT) payments to WAHSA's county nursing homes.
Maximum Payments for Direct Care Services Continue to Decline
Direct care costs include wages and benefits for nursing facility caregivers, including RNs, LPNs and CNAs. The nursing home payment formula establishes a maximum payment for direct care service costs and costs in six other cost centers. That maximum was set to cover the direct care costs of facilities at 103% of the statewide median in FY 1998-99. Despite a 2.5% rate increase under 1999 Act 9 for FY 1999-00, the direct care maximum dropped to 102.3% of the statewide median, one of the lowest levels in the country for states with cost-based reimbursement systems. According to the WAHSA database, 94 of 154 member facilities, or 61%, will not be fully reimbursed for their direct care costs despite the 2.5% rate increase provided under Act 9 . The 2% rate increase provided under Act 9 for FY 2000-01 most likely will result in further reductions in those direct care maximum payments.
Medicaid Labor Region Changes Could Cut Facility Rates
The 1999-00 nursing home payment formula implemented by DHFS included a significant change in the state labor region designations used to determine facilities' direct care rates. This change is generally based on the labor region designations utilized by the federal government to establish payments under the Medicare program. During the current biennium DHFS has agreed to phase-in the fiscal impact of switching to the new labor regions; however, it intends to fully transition to the new regions effective July 1, 2001. Without additional Medicaid funding in 2001-03, fully implementing the Medicare labor regions could be disastrous for some homes.
Although a number of homes stand to gain under this change, facilities in the following counties could receive a 2001-02 rate reduction under the Medicare labor regions: Adams, Columbia, Dodge, Fond du Lac, Grant, Green, Green Lake, Iowa, Jefferson, Juneau, Lafayette, Marquette, Polk, Richland, Sauk, Sheboygan and Walworth Counties . Some facilities are scheduled to drop from the current "high" labor region to Medicare's "rural" labor region. These homes could receive a direct care rate cut of $1.59 per resident/day, or for a facility with 100 Medicaid residents, an annual cut of $58,000, the salary and fringe equivalent for 2.5 full-time CNA positions. Facilities in Sheboygan County stand to fare even worse. Medicare has designated Sheboygan County as the lowest labor region in Wisconsin. A facility with 100 Medicaid residents in this county could receive a rate cut of $73,000, the wage and fringe equivalent for 3.4 CNA positions.
Transition to a Medicaid "Case-Mix" Reimbursement System
In July 2001, DHFS intends to begin transitioning to a new Medicaid nursing home reimbursement system. This new system will be similar to Medicare's nursing home Prospective Payment System which incorporates resident resource utilization groups (RUGs) to establish payment rates according to levels of care. Many other states have elected to convert their Medicaid payment systems to one based on Medicare's RUGs. Based on the experience of these states, however, it is obvious that transitioning to a RUGs-based system will require additional Medicaid funding. Numerous reports note that while the RUGs system somewhat effectively establishes levels of care reflective of nursing facility residents' medical needs, this system does not adequately assess, and therefore reimburse for, the needs of residents exhibiting challenging behaviors. In addition, transitioning to this new system will likely cause significant swings in reimbursement rates among nursing homes. In order to assure fiscal stability within Wisconsin's nursing homes during the transition to a RUGs payment system, additional Medicaid funding will be required.
Private Pay Rates Are Too High
Because Medicaid pays facilities rates that fall substantially below the actual cost of providing care and services, private pay residents are forced to subsidize the Medicaid program. According to the DHFS 1998 Annual Survey of Nursing Homes, the average skilled care rate paid by private pay residents was thirty-five percent higher than the rate paid by Medicaid (In 1998 the average private pay rate was $130/day, compared to a Medicaid rate of $96). If substantial 2001-03 Medicaid nursing home funding increases are not approved, this substantial subsidization of the Medicaid program by private pay residents will unfairly but undoubtedly continue to increase.
The State's Commitment to Funding Nursing Home Services Is Declining
Over the past decade, nursing home providers have sought and helped succeed in passing two wage pass-through proposals (and are seeking a third), a $32 dollar per occupied bed tax on its residents and the intergovernmental transfer program (IGT), which uses county nursing home deficits as the State share to capture matching federal Medicaid funds. Between the bed tax and the IGT, Wisconsin will be able to capture an additional $122 million in federal Medicaid funding this year. At the same time, however, State GPR funding for nursing homes has declined from $233.7 million in FY 1994-95 to a budgeted amount of $199.4 million in FY 2000-01, a drop of approximately 14.7% (see Table I).
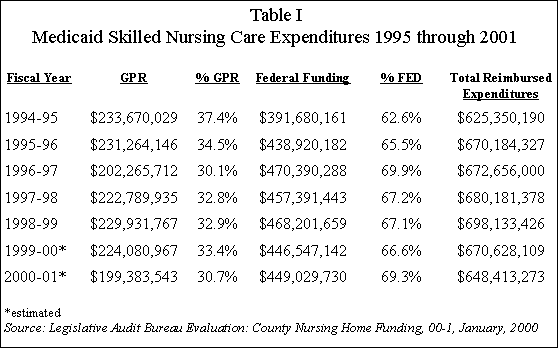
We are just about out of funding gimmicks and fiscal bandaids to offset the declining State GPR commitment to its nursing home residents and those who care for them.
The Solution
WAHSA members will seek to work with the Governor, the Legislature and the DHFS to develop a permanent and stable solution to the nursing home funding problem as part of the 2001-03 state budget.

The Wisconsin Association of Homes and Services for the Aging (WAHSA) is a statewide membership organization of not-for-profit corporations principally serving elderly and disabled persons. Membership is comprised of 190 religious, fraternal, private and governmental organizations which own, operate and/or sponsor 194 not-for-profit nursing homes, 71 community-based residential facilities, 39 residential care apartment complexes, 100 independent living facilities, and 446 community service programs which provide services ranging from Alzheimer's support, child day care, hospice and home care to Meals on Wheels. For more information, please contact the WAHSA staff at (608) 255-7060: John Sauer, Executive Director; Tom Ramsey, Director of Government Relations; or Brian Schoeneck, Financial Services Director.

WAHSA 204 South Hamilton Street Madison, WI 53703
Telephone: (608)255-7060 FAX:(608)255-7064









